In 2017, Republicans had a chance to “repeal and replace” Obamacare and quickly realized that they were going to have to replace it with either a) something terrible or b) something that looked a lot like Obamacare.
In 2021, some advocates are talking about repealing and replacing the Lanterman-Petris-Short Act—the “Magna Carta” for the mentally ill that has governed involuntary treatment in California since 1967. But the reality is that any replacement for LPS will either be a) unconstitutional or b) look a lot more like LPS than people seem to think. Any window for reform is likely to be short-lived, so we should think carefully about proposals that generate a huge amount of opposition without a lot of change (as seems to have been the case with SB1045).
In my own research, I’ve been highlighting ways in which the LPS system is failing clients, families, and clinicians. The system is byzantine and cumbersome, with distinctive pathways for people who are “danger to self” “danger to others” or “grave disability” (even though people, being people, are often a complex mix). Clinicians are often making evaluations based just on what they can see in front of them, without knowing what has and hasn’t worked in the past; they might even be barred from testifying to what they learn from family members or other providers in court. And throughout the system, decisions that everyone I talk to thinks should be made based on the delicate balance between civil liberties and welfare are actually driven by resource constraints and financial incentives.
Although I think some reforms are justified, there are four reasons why I think discussion of “repealing” LPS is a dead end.
First, there’s just not that much room for variation in the statute or commitment process. The Treatment Advocacy Center, which advocates for expanding forced treatment as a way to address homelessness and incarceration among people living with severe mental illness, gives California a “D-” for its commitment laws. This means less than it might seem. The state ranks poorly mostly because only professionals, not families or concerned citizens, can petition courts to hospitalize someone. The “grave disability” standard, on which many proposals for reform are centered, is ranked as being as well-written as the statute in Minnesota, which received an “A+”.
No matter what reform California implements, the Supreme Court’s O’Connor vs. Donaldson decision, which declares that states may not confine a non-dangerous person “capable of surviving safely in freedom,” will stand. There is no prospect of returning to the old standard that prevailed pre-LPS of hospitalizing those “who are of such mental condition that they are in need of supervision, treatment, care or restraint.” And, given that the investigation that led to LPS discovered that this standard led to “Senior citizens being shoveled into hospitals…by many thousands a year,” we probably wouldn’t want to anyway. States do have different time periods and procedures for commitment, but the basic architecture and requirements are the same across the U.S.
The second problem is with the narrative among advocates, particularly family members, that involuntary hospitalization, as a medical treatment for a medical condition, should be purely a medical decision, and that laws like LPS throw needless procedural and legal roadblocks in the between illness and treatment. The idea that mental illness should be treated as an “illness like any other” is a powerful talking point for challenging discrimination and stigmatization. But it isn’t true. Yes, doctors can intervene in some circumstances on a patient who is unconscious or with dementia without their consent. But mental illness is the only domain where we routinely impose treatment against someone’s explicitly stated preferences. And, given that, judges are going to continue to have their say. Even France, a country that held out until 2011 against systematic judicial review of hospitalizations, has given in under a barrage of human rights complaints and exposés of abuse.
Third, it’s not clear that changing the law would matter that much, particularly if the goal of reform is to obligate more people into treatment. We have very little data about involuntary commitments in the U.S. But a recent study on the states that do publish rates of involuntary hospitalizations doesn’t suggest that looser laws will lead to more hospitalizations. Michigan (“A” by TAC’s grading) has about one-fifth as many involuntary holds per year as Florida (“D”). This non-linkage holds internationally. A study of European countries found no statistically significant relationship between rates of involuntary hospitalizations and the laws in place.
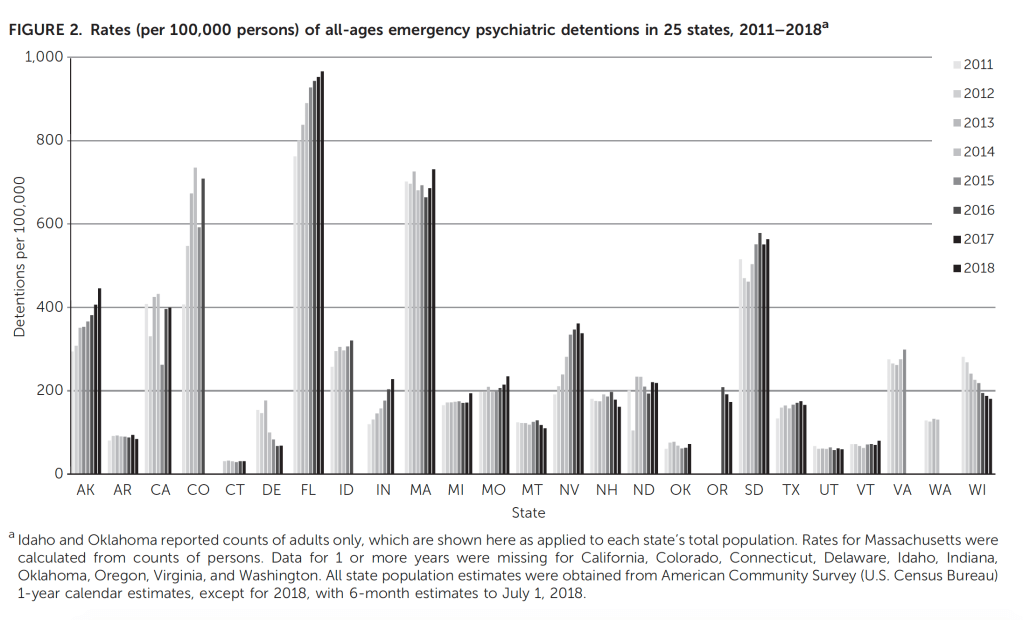
Source: Lee, Gi, and David Cohen. 2020. “Incidences of Involuntary Psychiatric Detentions in 25 U.S. States.” Psychiatric Services appi.ps.201900477. doi: 10.1176/appi.ps.201900477.
The factors that determine who gets involuntary care are systemic, not statutory. As I’ve been harping on in my report, in practice criteria like “grave disability” are interpreted as something akin to “whatever fills available beds.” You could alter the standard to say that homelessness is, by itself, a criterion for involuntary internment. But it wouldn’t change much: the beds are full, the reimbursement rates are low, and for-profit private hospitals are still going to have all the incentive in the world not to focus on complex, non-consenting patients.
And this leads to my fourth point. Focusing on the law is a dead end if it distracts us from reorganizing the system in a way that matches peoples’ needs. Reforms to regulations like the IMD exclusion, which bars MediCaid funds from going to certain kinds of psychiatric hospitalizations, are more technical but also more impactful (and therefore should be considered with maximum caution). They force us to think beyond the idea of “people not getting treatment should be put into treatment” to where and what treatment is likely to meet peoples’ needs and, perhaps, even be something people might want.
53 years on, I truly believe LPS is still something California should be proud of. It was a worldwide model for what one report described as a “revolution against violence” in psychiatry. Most people discussing the bill’s aims mention the first goal stated in its preamble: to end the inappropriate, indefinite, and involuntary commitment of persons with mental health disorders.” It largely did.
But the Bill’s aspirations actually went much further: “b) To provide prompt evaluation and treatment,” “c) to guarantee and protect public safety,” “d) to safeguard individualized treatment,” “e) to provide individualized treatment, supervision, and placement services,” “f) to encourage the full use of all existing agencies, professional personnel, and public funds to accomplish these objectives,” and “g) to protect persons with mental health disorders…from criminal acts.”
We might want to tweak “a)” and then face up to the more difficult work of implementing “b)” through “g).”